- Why so much controversy?
- Airborne transmission
- RCTs of masks – strengths/limitations, community, healthcare settings
- Meta-analyses – gold standard or lazy lumping?
- Non-RCT evidence – why is it needed, what does it show?
- AOB
https://twitter.com/trishg...
First, ‘masks’ and ‘masking’ are very broad terms. They cover different technologies (cloth, medical, respirator), wearers (public, patient, healthcare worker), settings (low v high risk) and requirements (mandated v free choice).
Because of this multiplicity, statements like “masks [don’t] work” may be referring to very different interventions in different populations for different activities at different times, not to mention different diseases. The literature, in short, is a mess.
Second, masking is a cultural practice as well as a public health intervention. It has symbolic meaning. Pirates and burglars wear masks. To some, masking means you’re a ‘pansy’, ‘sheep’ etc. Masking offends libertarians.
https://www.bmj.com/conten...
There’s strong social pressure to mask in some settings to contribute to the greater good (“my mask protects you”). People may feel pushed into doing something which a) feels awkward, b) symbolises an allegiance they don’t identify with and c) they feel is ineffective.

Face coverings for covid-19: from medical intervention to social practice | The BMJ
Helene-Mari van der Westhuizen and colleagues argue that face coverings should be considered not as medical equipment but as a social practice informed by norms and expectations ### Key messages Covering the mouth and nose is a public health measure designed to capture respiratory droplets from th..
Third, masking (whatever its benefits) has some downsides. It’s (depending on the design) uncomfortable. It can interfere with communication (especially if hard of hearing). If you work long shifts, it gets hot/sweaty behind the mask.
https://www.bmj.com/conten...

Face masks can be devastating for people with hearing loss | The BMJ
Innovation is urgently needed to ensure clear communication in medical settings The covid-19 pandemic has literally changed the face of medical care: clinicians, nurses, other staff, and patients are all wearing masks. We are trying to communicate while keeping the required distance apart. With mas..
In short, masking is something many of us feel strongly about. It’s not even possible to separate “the science” of masks from “the politics”, since science does not sit in some protected bubble away from the rest of society. Read on!
Understanding why & to what extent masks work requires knowledge of how the SARS-CoV-2 virus is transmitted. With colleagues, I published this summary of evidence that it spreads *predominantly* via air. https://twitter.com/trishg...
I responded to critics of that paper here https://twitter.com/trishg... (plus see more in thread below).
For those who want depth and detail, here’s Chia Wang and team’s stunning review of the evidence for airborne transmission in Science (one of the very top scientific journals).
https://www.science.org/do...
In sum, it is *settled science* that SARS-CoV-2 is transmitted via the air. Settled, that is, in all branches of science *except* key groups of doctors, including some in powerful positions at the World Health Organisation. I’ll return to that paradox later.
Medical/surgical (~same thing) masks are designed to stop spatter (e.g. your dentist dribbling into your mouth). Most aren’t made to a specific quality standard. Respirators are designed to filter out airborne particles. They ARE made to a standard.
If SARS-CoV-2 were spread mainly by droplets, we’d need to focus on handwashing and medical/surgical masks which stop wet drops. If mainly via the air, we need to focus on air quality and use the kind of face coverings that stop airborne particles (i.e. respirators).
All masks stop some airborne particles (even if the holes are bigger than the particles, fibres are criss-crossed and electrostatic forces kick in). But N95 (FFP2) respirators stop >95% of particles of SARS-CoV-2 size, and N99s (FFP3s) stop >99%.
A year ago, we wrote this article recommending that everyone upgrades their mask from either medical/surgical to respirator.
https://theconversation.co...
Whilst respirators protect best, ANY mask is better than none. Efficiency at reducing transmission of respiratory aerosol:
N95 respirator 99%
Medical mask 59%
Bandana (single) 47% (double) 60%
Face shield 2%
https://tandfonline.com/do...
The above, a laboratory study of artificial aerosols, should not be taken as direct evidence that these masks would be this effective/ineffective in preventing real-world SARS-CoV-2 transmission. But they *add to the mix of evidence*. More on that later.
Face shields are only 2% effective cos they’re designed to stop spatter, NOT filter air. Medical masks don’t fit snugly, so instead of breathing filtered air, you breathe what leaks in round the sides. This is why a doubled-over bandana works pretty well!
While I believe cloth/medical masks have a place, some sfeel the benefits of respirators are so great, we should junk all lesser kinds of masking.
https://www.cidrap.umn.edu...
Remember, respirators (and masks) only work if they fit you snugly. You don’t need a professional fitting any more than you need to have your underwear professionally fitted, but do check for gaps.
RCTs of masks have continued to generate more heat than light. I’m going to reproduce what I said two years ago, which still holds (even more so now, since what has happened since could have been predicted from my earlier thread).
In the name of evidence-based medicine (EBM), the West got off on the wrong foot. We became obsessed with the holy grail of a definitive randomised controlled trial (RCT) that would quantify both the benefits and the harms of masks, just as you would for a drug.
If you were raised in the EBM tradition, where “rigorous RCTs” are mother’s milk, it’s not easy to get your head round why this was a bad way to approach the problem. Looks like Prof G has lost it, dropped her standards, joined the dark side etc. Bear with me.
A RCT is a controlled experiment. Since people are randomly allocated to one or other group (‘arm’), any confounding variables are distributed evenly between the arms so they all cancel out (so long as the study is large enough and allocation is truly random).
Random allocation means that differences between the arms of a RCT are highly likely to be due to the intervention (in this case, masks) and not to confounders. But it doesn’t follow that a RCT is better, for any scientific question, than a non-RCT design. Why not?
Many reasons. Drugs are (arguably) a simple intervention, but masks are a highly complex one. There are two key questions: do they protect the wearer from other people’s germs – and do they protect other people from the wearer’s germs (‘source control’)?
The RCT design can’t (usually) cope with this. It’s easy to design a study where the main outcome is infection in wearers, but how would a RCT of source control work? Answer: do an enormous study to randomise entire towns to either masking or not masking!
Impressively, jabaluk and team did just this. They randomised 600 villages in rural Bangladesh (over 300,000 people) to getting free masks (‘interventions’) or not (‘controls’). For 2 months, they observed mask-wearing and counted covid-19 cases in all villages.
The Abaluk RCT was published in Science (really top-notch academic journal). It showed that in the intervention villages, a) mask wearing was three times as high as in the control villages, and b) incidence of covid-19 was lower.
https://www.science.org/do...
Despite the large size of the Bangladesh RCT, differences in covid-19 incidence were relatively modest and only just reached statistical significance when measured by blood test. Differences were greater where surgical rather than cloth masks were used.
Does this mean “masks don’t work” in the community? NO! Looks like even in free-living conditions (people can choose not to wear), they have a modest but important effect—reducing transmission by around 10%. Let me return to some of the arguments I put out two years ago.
For policy decisions, we’re not just interested in whether masking reduces community incidence of covid-19 during a short intervention period (say, a month or two). We’re interested in how masking impacts on the *exponential spread* of an accelerating pandemic.
Take the number 1, double it, then keep going. 1 becomes 2, then 4, etc. After 10 doubles, you get 512. After 10 more doubles, 262144. Now instead of doubling, multiply by 1.9 (a tiny reduction in growth rate). After 20 cycles, the total is only 104127.
=> if masks reduce transmission by a TINY bit (too tiny to be statistically significant in a short RCT), population benefits are still HUGE. If instead of doubling every 9 days, covid rates increased by 1.9 every 9 days, after 180 days cases would be down by 60%.
These two issues—the near-impossibility of using RCTs to test hypotheses about source control and over-reliance on “statistically significant effects” within a short intervention period—is why a RCT of masks is *highly likely to mislead us*.
Let’s look at the other big community-based RCT of masks in covid-19. The *big Danish mask trial* became one of the most talked-about RCTs in the pandemic. Its main finding was negative (no significant impact of masks compared to no masks).
https://www.acpjournals.or...
But the DANMASK RCT was *fatally flawed* as
dgurdasani1
and I argued here. I’ll summarise in the next tweet. https://spectator.co.uk/ar...
DANMASK RCT flaws: no CONSORT statement, no ethical approval, inappropriate setting (there was almost no Covid circulating at the time!), under-powered sample, wrong primary outcome, wrong intervention period, inaccurate test, misinterpretation of own findings.
There *never will be* RCT evidence to definitively answer the question “do masks work in community settings?”, because RCTs can’t generate dynamic evidence to understand complex social interventions in diverse and changing contexts. Answer will always be “to some extent”.
The question of how to protect HCWs is politically contentious, since it involves the sensitive topic of occupationally-acquired disease and the risk (in rare but well-described cases) of a HCW dying from covid-19 caught at work.
Broadly speaking, HCW unions want high-grade protection for their members; employers want to spend as little as possible on personal protective equipment (PPE). So RCTs comparing medical masks (cheap) with respirators (more expensive) have particular significance.
There’s been only one published peer-reviewed RCT of masking in HCWs during covid-19. Loeb et al did a 5-country study which showed no statistically significant difference between medical masks and respirators:
https://pubmed.ncbi.nlm.ni...
The Loeb study has been heavily criticised. I have two major concerns. First, according to the original study protocol, HCWs were asked to wear the mask/respirator “when providing routine care to patients with COVID-19 or suspected COVID-19”.
Because SARS-CoV-2 is airborne (see tweets 9-20), removing masks when not in the close vicinity of known or suspected covid patients is illogical. See why we need to understand the mode of transmission to interpret the studies?
Even though the words quoted in tweet 42 are taken directly from their participant information sheets, Loeb and colleagues say that participants were “expected” to wear their mask or respirator all the time when at work.
There is confusion about which participants wore what and when in the Loeb RCT. This may not be entirely the authors’ fault, as the study was occurring in a changing policy context (universal masking of HCWs came and went in some sites as the trial progressed).
My other concern with the Loeb RCT is that results are heavily skewed by data from Egypt, the largest national subsample. There was a big wave of Omicron in Egypt at the time, so HCWs in both arms could well have caught the virus outside work.
Even if Egyptian HCWs wore their protection all the time at work, if they then went home and played with their infected kids, they’d be as likely to catch covid as anyone else. Egypt was the only country where *more* infections occurred in the respirator arm!
Loeb et al are currently responding to these and other methodological criticisms. ONE explanation for their findings is that respirators are no more effective than medical masks. Another is that a benefit exists but this trial failed to demonstrate it.
You may have seen recent headlines that a Cochrane review demonstrated a lack of RCT evidence for efficacy of masks. Here’s the review so you know what I’m criticising. I don’t endorse it.
https://www.cochranelibrar...
Despite widespread claims that this new meta-analysis (actually, an update of an old meta-analysis) has definitively demonstrated that “masks don’t work” in reducing covid-19 transmission, it doesn’t show anything of the sort. Let me explain.
Of 78 studies in this Cochrane review, only 6 (2 on masks) were done in the pandemic. The rest were in earlier (less contagious) outbreaks e.g. flu.
https://www.vox.com/future...
As well as combining covid studies with non-covid studies, Jefferson et al made another elementary lumping error. They combined RCTs in which HCWs had worn protection *some of the time* with RCTs in which they wore them *all the time*.
A meta-analysis combining different studies asking different Qs will tend to produce un-nuanced & often negative findings. Mixing paints in a paintbox gives brown.
https://theconversation.co...
Here, JenniferNuzzo points out additional subtleties that cast doubt on the masks-don’t-work conclusion (which is not in any case what the authors of the review concluded—at least, not in the review itself).
https://twitter.com/Jennif...
Here, Jason Abaluk jabaluk of the impressive Bangladeshi mask RCT argues that the updated Jefferson review made the same mistakes they had made in previous versions.
https://twitter.com/Jabalu...
Here, Satoshi Akima @ToshiAkima explains why Cochrane reviews should not be blithely swallowed as an assumed ‘gold standard’.
https://twitter.com/ToshiA...
Satoshi argues that whilst RCTs may provide *predictive* evidence (intervention A is more/less likely to produce outcome X than intervention B), they don’t provide *mechanistic* evidence (how does intervention A work?). I’ll come back to this.
Here, DanWalker9999, citing BlakeMMurdoch, accuses authors of the Jefferson Cochrane review of “amazing sloppiness” (failing to access and incorporate raw data from Abaluk RCT that was in the public domain).
https://twitter.com/danwal...
Have I persuaded you that Cochrane reviews aren’t a magical higher form of science that automatically knocks all other evidence out of the park? They look at a narrow slice of evidence and can be done well or badly. Where’s the quality control? Good question.
Some (though not all) Cochrane authors believe that the RCT is such a superior form of evidence that we don’t even have to look at any other kinds of evidence (unless our search for RCTs turns up none). Let me explain why this is a dangerously naïve assumption.
Bradford Hill (famous for doing the 1st ever RCT) emphasised that we can’t rely solely on probabilistic evidence from RCTs. We also need mechanistic evidence (see tweet 58). We explain in this paper on EBM+:
https://ebm.bmj.com/conten...

Adapt or die: how the pandemic made the shift from EBM to EBM+ more urgent | BMJ Evidence-Based Medicine
Evidence-based medicine (EBM’s) traditional methods, especially randomised controlled trials (RCTs) and meta-analyses, along with risk-of-bias tools and checklists, have contributed significantly to the science of COVID-19. But these methods and tools were designed primarily to answer simple, focuse..
When Jefferson et al ignore ALL evidence except RCTs and also use synthesis methods that *make no sense* when you take the *mechanism of transmission* into account (i.e. lumping continuous masking RCTs with intermittent masking RCTs), I have a problem.
Mechanistic evidence (which Jefferson et al conspicuously ignore) means evidence – from basic science laboratory experiments and real-world case studies for example – that helps us understand how the virus spreads and how covering the face *could* work.
Airborne transmission happens *mainly* when you’re very close to someone who is exhaling the virus. But airborne viruses *float in the air* so they spread throughout an indoor space. Rules like “wear your mask/respirator within 2 metres” don’t make sense.
Airborne transmission of SARS-CoV-2 explains why protection that *blocks airborne particles* (i.e. respirators) is in theory better than protection that blocks droplets, and why we’d expect a well-designed RCT of respirators vs masks to show an advantage of the former.
Just because mechanistic evidence suggests that respirators will outperform medical masks doesn’t mean we should ignore results of RCTs that show no advantage. But it does mean we should *design those RCTs properly* so that an advantage, if it exists, would show up.
Because RCTs and meta-analyses were poorly designed (overlooking mechanism of transmission), many produced negative findings. Some researchers (+ press and public) have conflated *absence of evidence of effect* with *evidence of lack of effect*.
I’ve argued from a philosophical perspective that flawed mental models of how SARS-CoV-2 spreads led scientists to vastly under-estimate the importance of masking. (NB I’m NOT saying it’s bad to wash hands) (https://royalsocietypublis...
For a long time, WHO and other bodies denied that SARS-CoV-2 was airborne (see tweets 9-20). We wrote a paper on why this error happened (TL;DR: powerful people had entrenched mental models + reputations to lose). https://wellcomeopenresear...
These flawed mental models led to flawed policy narratives, diverting us into an *obsessive concern with handwashing and squirty sanitisers* and thinking that medical masks (designed to block droplets) will do for HCWs.
https://www.bmj.com/conten...

How covid-19 spreads: narratives, counter narratives, and social dramas | The BMJ
Trisha Greenhalgh and colleagues explore why inaccurate narratives about the mode of transmission of SARS-CoV-2 emerged early in the pandemic and shaped a flawed policy response, with tragic consequences ### Key messages The draft terms of reference for the UK covid-19 inquiry encompass not just w..
Let’s return to the question of community masking. Notwithstanding jabalok’s impressive RCT, it remains the case that this kind of study is difficult and expensive to do and hard to interpret. What other evidence is there? I get asked this question a lot.
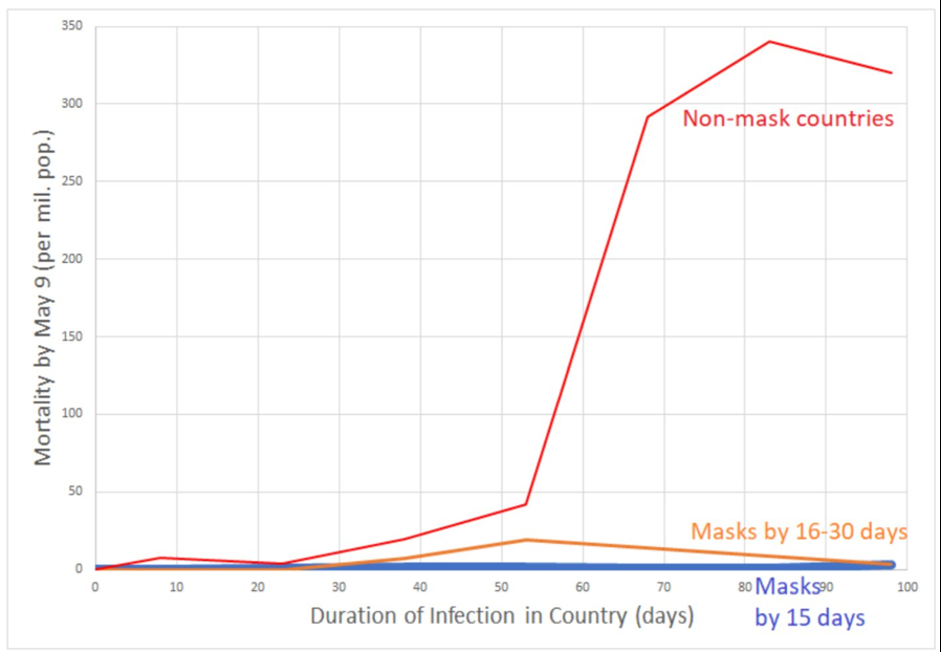
Countries that introduced mandated masking within 30 days of the first case (mostly Asian) had *dramatically* fewer Covid-19 cases than those that delayed beyond 100 days (mostly Western).
https://ajtmh.org/view/jou...
Was this association or causation? Early on, we didn’t know (though, importantly, nobody in these Asian countries seemed to come to harm from wearing a mask). Since that early study, there have been numerous studies of the impact of mask mandates.
Various systematic reviews of mask mandates have been published. This one showed a statistically significant effect of mask mandates (same effect size as handwashing, with physical distancing having an even greater effect)
https://www.bmj.com/conten...

Effectiveness of public health measures in reducing the incidence of covid-19, SARS-CoV-2 transmission, and covid-19 mortality: systematic review and meta-analy..
Objective To review the evidence on the effectiveness of public health measures in reducing the incidence of covid-19, SARS-CoV-2 transmission, and covid-19 mortality. Design Systematic review and meta-analysis. Data sources Medline, Embase, CINAHL, Biosis, Joanna Briggs, Global Health, and World ..
Li et al did a meta-analysis of case-control studies. Acknowledging the limitations of such designs, they found that masks reduced SARS-CoV-2 infections by (on average) ~70% in healthcare workers and ~60% in lay people
https://ncbi.nlm.nih.gov/p... 3
What’s a case-control study? Find people who caught Covid and match them with people who were similar but didn’t catch Covid; ask whether each was wearing a mask. Relatively weak design (bc unmeasured confounders), but not as weak as a badly-designed RCT.
A review of observational studies of public health measures in the pandemic found 6/7 studies of mask mandates showed statistically significant effects. Studies rated higher quality found greater effects.
https://www.sciencedirect....
This study by Liu et al looked at (among other things) the introduction of mask mandates across different US states. After correcting for confounders, they estimated mask mandates reduced transmission by 29%.
https://link.springer.com/...

Differential impact of non-pharmaceutical public health interventions on COVID-19 epidemics in the United States | SpringerLink
The widespread pandemic of novel coronavirus disease 2019 (COVID-19) poses an unprecedented global health crisis. In the United States (US), different state governments have adopted various combinations of non-pharmaceutical public health interventions (NPIs), such as non-essential business closures..
A recent study of observational data across different US states showed that (after complex statistical measures to correct for confounders) mask mandates were associated with significantly reduced transmission rate.
https://bmjmedicine.bmj.co...

Non-pharmaceutical interventions and covid-19 burden in the United States: retrospective, observational cohort study | BMJ Medicine
Objective To evaluate the adoption and discontinuation of four broadly used non-pharmaceutical interventions on shifts in the covid-19 burden among US states. Design Retrospective, observational cohort study. Setting US state data on covid-19 between 19 January 2020 and 7 March 2021. Participants..
2 new studies of mask mandates in US states. Localities with mask mandates had lower transmission while mandates were in place & lower hospitalisations from covid-19
https://www.ncbi.nlm.nih.g...
https://www.ncbi.nlm.nih.g...
Here’s Miriam Van Dyke’s study of more granular data on mask mandates across the state of Kansas, USA, in 2020. Again, localities that implemented mask mandates had lower transmission after confounders controlled for.
https://www.ncbi.nlm.nih.g...
Cooper et al demonstrate that the association between mask mandates & lower covid-19 cases is causal.
https://www.sciencedirect....
We wrote a summary review of masks and masking here (now somewhat out of date but includes a lot of useful papers)
https://www.acpjournals.or...
The rest of this thread links to additional key evidence on the mask/masking debate. This from jljcolorado on why people wrongly assumed for so long that respiratory illnesses are droplet-spread.
https://twitter.com/jljcol...
A landmark paper from Adriaan Bax’s team showing that breathing, speaking and singing are key activities that transmit SARS-CoV-2 https://www.ncbi.nlm.nih.g...
The Bagheri et al modelling study: what if one person masks? What if both people mask?
https://twitter.com/Huffma...
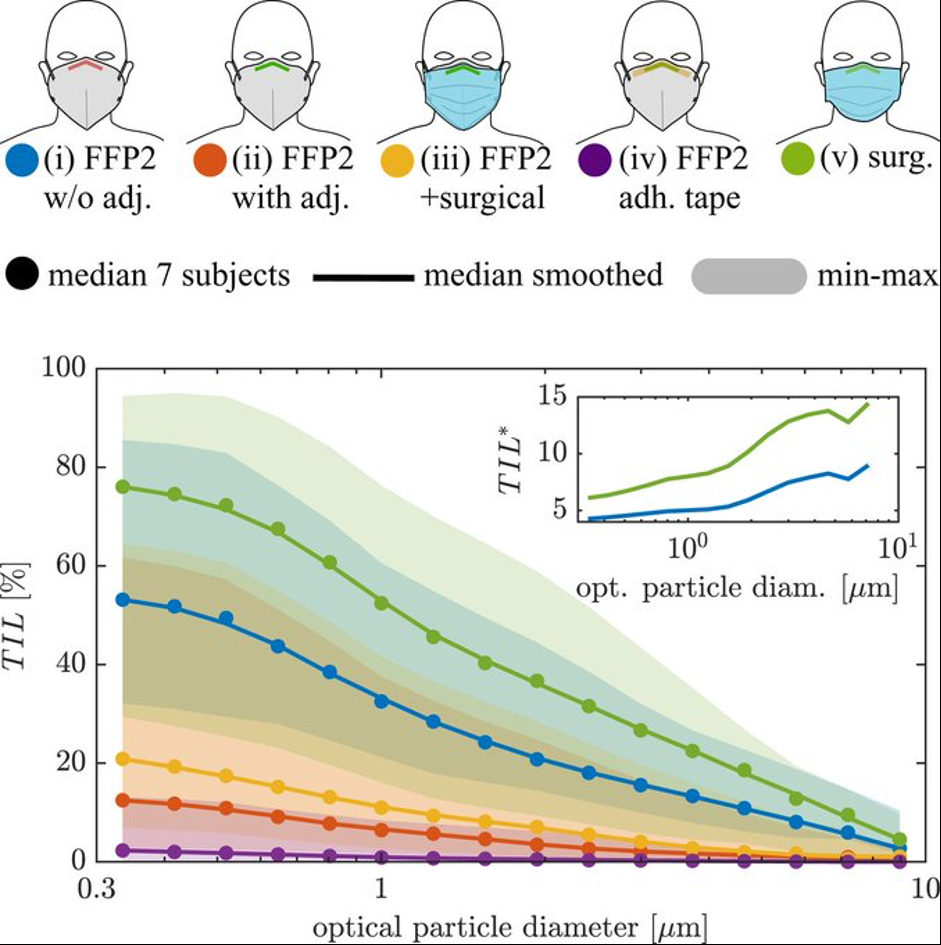
TIL = total inward leakage (vertical axis). This is jargon for "air getting in round the sides of your badly-fitting mask". High TIL is bad. Aim for PURPLE: wear FFP2 & use tape to close gaps. GREEN is untaped surgical mask - useless! https://www.pnas.org/doi/p...
Here’s a nice theory-based review of the psychology of mask-wearing (or mask-refusing). Talks about 3 main constructs: autonomy, psychological relatedness, and competence.
https://www.mdpi.com/1660-...

IJERPH | Free Full-Text | Commentary: Physiological and Psychological Impact of Face Mask Usage during the COVID-19 Pandemic
In this commentary, we discuss the physiological effects of wearing masks for prolonged periods of time, including special considerations, such as mask wearing among those who engage in exercise training, and concerns for individuals with pre-existing chronic diseases. In healthy populations, wearin..
Thanks several people for pointing out I forgot to add the before-and-after Cambridge study showing HCW covid infections went right down after N95s introduced
https://www.cam.ac.uk/rese...
We don't have to wear masks everywhere, for ever. We should adjust our masking behaviour to reflect the prevailing risk of transmission.
https://theconversation.co...